The Influenza (Flu) Virus
Next to the common cold, influenza or "the flu" is perhaps the most familiar respiratory infection in the world. In the United States alone, approximately 25 to 50 million people contract influenza each year. The symptoms of the flu are similar to those of the common cold, but tend to be more severe. Fever, headache, fatigue, muscle weakness and pain, sore throat, dry cough, and a runny or stuffy nose are common and may develop rapidly. Gastrointestinal symptoms associated with influenza are sometimes experienced by children, but for most adults, illnesses that manifest in diarrhea, nausea, and vomiting are not caused by the influenza virus though they are often inaccurately referred to as the "stomach flu." A number of complications, such as the onset of bronchitis and pneumonia, can also occur in association with influenza and are especially common among the elderly, young children, and anyone with a suppressed immune system.
Influenza is highly contagious and is more common during the colder months of the year. Contrary to traditional belief, however, the climate itself is not directly to blame for the increase in incidence, but rather is attributable to the greater amount of time spent indoors in close proximity to other individuals during inclement weather. The influenza virus is chiefly transmitted through airborne respiratory secretions released when an infected individual coughs or sneezes. Incubation typically is from one to two days from the time of infection, and most people begin to naturally recover from symptoms within a week. The vast majority of influenza-related deaths are caused by complications of the flu rather than the actual influenza virus.
Three distinct types of influenza virus, dubbed A, B, and C, have been identified. Together these viruses, which are antigenically distinct from one another, comprise their own viral family, Orthomyxoviridae. Most cases of the flu, especially those that occur in epidemics or pandemics, are caused by the influenza A virus, which can affect a variety of animal species, but the B virus, which normally is only found in humans, is responsible for many localized outbreaks. The influenza C virus is morphologically and genetically different than the other two viruses and is generally nonsymptomatic, so is of little medical concern.
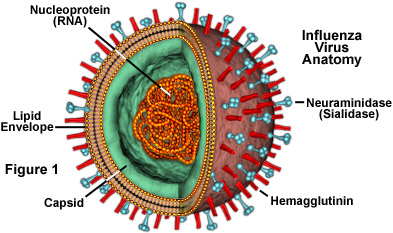
The structure of the influenza virus (see Figure 1) is somewhat variable, but the virion particles are usually spherical or ovoid in shape and 80 to 120 nanometers in diameter. Sometimes filamentous forms of the virus occur as well, and are more common among some influenza strains than others. The influenza virion is an enveloped virus that derives its lipid bilayer from the plasma membrane of a host cell. Two different varieties of glycoprotein spike are embedded in the envelope. Approximately 80 percent of the spikes are hemagglutinin, a trimeric protein that functions in the attachment of the virus to a host cell. The remaining 20 percent or so of the glycoprotein spikes consist of neuraminidase, which is thought to be predominantly involved in facilitating the release of newly produced virus particles from the host cell. On the inner side of the envelope that surrounds an influenza virion is an antigenic matrix protein lining. Within the envelope is the influenza genome, which is organized into eight pieces of single-stranded RNA (A and B forms only; influenza C has 7 RNA segments). The RNA is packaged with nucleoprotein into a helical ribonucleoprotein form, with three polymerase peptides for each RNA segment.
Mutations in the antigenic structure of the influenza virus have resulted in a number of different influenza subtypes and strains. Specific varieties of the virus are generally named according to the particular antigenic determinants of hemagglutinin (13 major types) and neuraminidase (9 major types) surface proteins they possess, as in influenza A(H2N1) and A(H3N2). New strains of the influenza virus emerge due to a gradual process known as antigenic drift, in which mutations within the virus antibody-binding sites accumulate over time. Through this mechanism, the virus is able to largely circumvent the body's immune system, which may not be able to recognize and confer immunity to a new influenza strain even if an individual has already built up immunity to a different strain of the virus. Both A and B influenza viruses continually undergo antigenic drift, but the reformulation of influenza vaccines each year often enables scientists to take into account any new strains that have emerged.
Influenza A also experiences another type of mutation called antigenic shift that results in a new subtype of the virus. Antigenic shift is a sudden change in antigenicity caused by the recombination of the influenza genome, which can occur when a cell becomes simultaneously infected by two different strains of type A influenza. The unusually broad range of hosts susceptible to influenza A appears to increase the likelihood that this event will occur. In particular, the mixing of strains that can infect birds, pigs, and humans is thought to be responsible for most antigenic shifts. Notably, in some parts of the world, humans live in close proximity to both swine and fowl, so that human strains and bird strains, may readily infect a pig at the same time, resulting in a unique virus. New subtypes of influenza A develop abruptly and unpredictably so that scientists are unable to prepare vaccines in advance that are effective against them. Consequently, the emergence of a new subtype of the virus can cause a global pandemic in a very short amount of time.
In addition to vaccines, a few other weapons have been designed to combat the flu. The antiviral medications amantadine and rimantadine can help reduce severity of illness in individuals with influenza that begin utilizing the drugs within two days of the onset of symptoms. These drugs work by hindering the change in pH that is necessary for the flu virion to release its contents into the cytosol of a host cell. Two additional antiviral drugs, zanamavir and oseltamivir, are effective against both A and B types of influenza. Instead of interfering with pH shifts, zanamavir and oseltamivir block the glycoprotein neuraminidase so that the release of new virus particles is inhibited and their spread is thwarted. It is important to note that antibiotics are not capable of fighting the influenza virus itself, but are sometimes given to patients with the flu to stem attacks of opportunistic microorganisms that are responsible for many influenza complications.
Though widespread familiarity with the flu makes it seem relatively benign to much of the general population, the virus can be devastating. In 1918 and 1919, more than 20 million people died from a strain of the virus commonly known as the Spanish flu that circulated through almost all inhabited regions of the globe. Many other outbreaks have occurred since that time, though none have been as deadly. Nevertheless, influenza together with complications of the virus is consistently among the top ten common causes of death in the United States, ranking higher than some other much more widely publicized killers, such as the HIV virus that causes AIDS.
